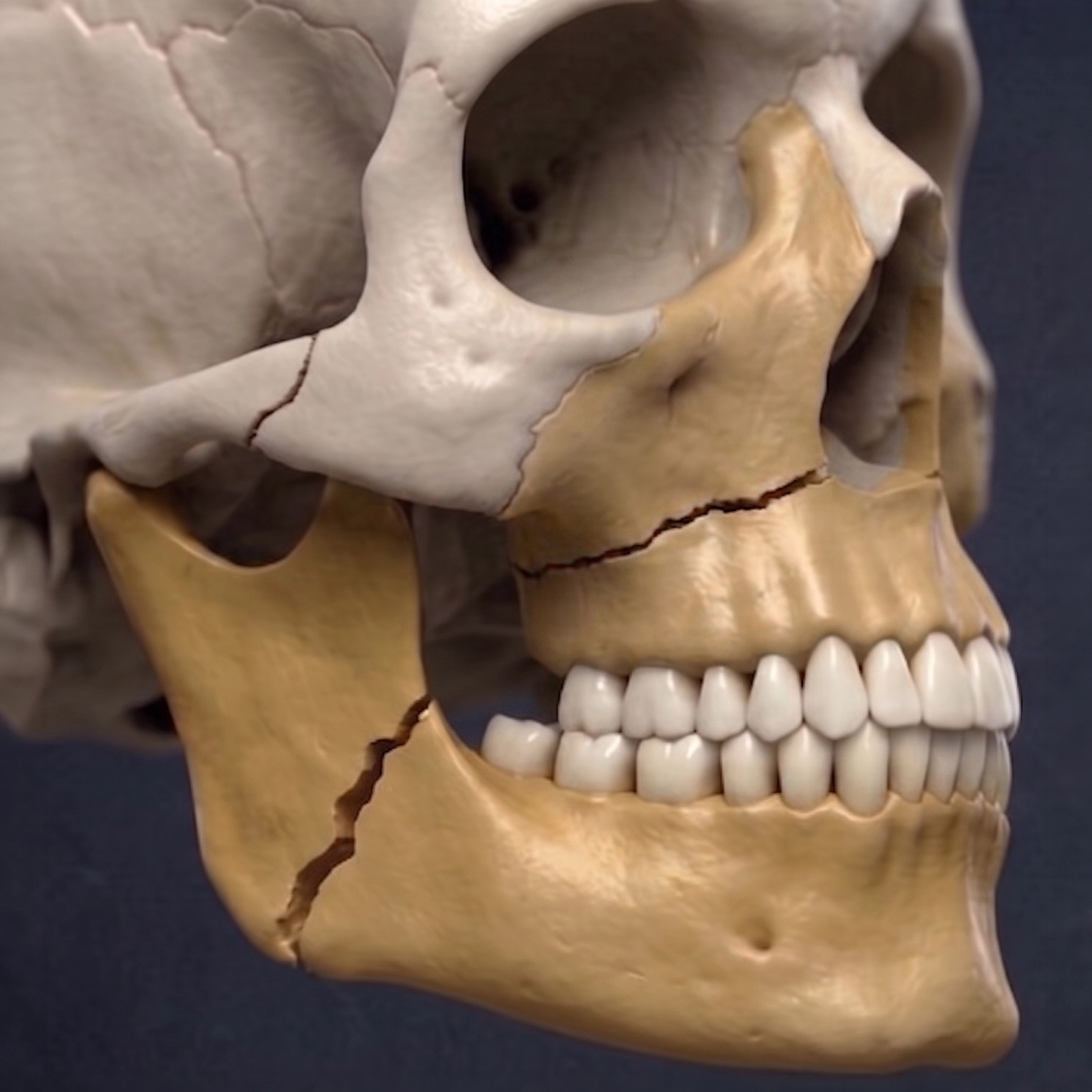
Broken Jaw (Jaw Fracture): Symptoms, Treatment and Recovery for Lower and Upper Jaw Injuries
Dr Varun Harish, FRACS Plastic Surgeon
First published:
A broken jaw is a fracture of the lower jaw (mandible), the upper jaw (maxilla), or both. This forms part of a broader group of injuries known as facial fractures, which can affect different parts of the face and vary in severity. Most people use the term to refer to the lower jaw, but the upper jaw can also be injured and is often overlooked.
The most important sign of a broken jaw is a change in the bite, where the teeth no longer meet the way they normally do.
Jaw fractures can affect chewing, speaking, mouth opening, and facial stability. Lower jaw fractures are often noticed because the bite feels wrong, the jaw is painful to move, or the lower lip or chin becomes numb. Upper jaw fractures may cause a changed bite, pain in the upper jaw or cheek area, or a feeling that the upper jaw is loose or moving when it should not.
Some jaw fractures are stable and can heal without surgery. Others need treatment to restore alignment, bite, and function.
 At a glance
At a glance
- A broken jaw can involve the lower jaw (mandible), the upper jaw (maxilla), or both.
- One of the most important warning signs is a new bite change.
- Pain with chewing, mouth opening, or speaking can all suggest a jaw fracture.
- Lower jaw fractures may cause lower lip or chin numbness.
- Upper jaw fractures may cause mobility of the upper jaw or midface.
- Some fractures heal without surgery.
- Displaced (bone ends have shifted) or bite-altering fractures are more likely to need surgery.
When to seek urgent medical care
Seek urgent assessment after facial trauma if you have:
- difficulty breathing
- heavy bleeding in the mouth
- an inability to bring your teeth together normally
- severe pain with inability to open the mouth
- loose or clearly mobile parts of the jaw
- a feeling that the upper jaw or middle of the face moves
- rapidly increasing swelling
- new numbness of the lower lip or chin
- major facial trauma with associated eye, nose, or head symptoms
Jaw fractures are not always dramatic in appearance. A person may have no obvious deformity but still have a clinically important injury if the bite has changed or part of the jaw is unstable.

Who Treats a Broken Jaw?
A broken jaw is treated by surgeons trained in facial trauma and jaw reconstruction. This may include plastic and reconstructive surgeons as well as oral and maxillofacial surgeons, depending on the injury and the healthcare setting.
In major trauma centres, these injuries are managed by surgical teams experienced in facial fractures, bite alignment, and reconstruction of the jaw and surrounding facial structures.
What matters most is not the title alone, but whether the surgeon has experience managing:
- jaw fractures affecting the bite and tooth alignment
- displaced (bone ends have moved out of alignment) or unstable fractures
- injuries involving both the lower jaw (mandible) and upper jaw (maxilla)
- more complex cases requiring jaw reconstruction
These injuries are not just broken bones — treatment focuses on restoring bite, function, appearance and facial stability. In more complex cases, this overlaps with the same principles used in jaw reconstruction after major cancer surgery. For this reason, surgeons who routinely manage complex facial trauma and perform jaw reconstruction, particularly in hospital-based multidisciplinary settings, are typically best equipped to treat these injuries.
How Do Jaw Fractures Occur?
Jaw fractures usually result from a direct force to the face or jaw. The pattern of injury often depends on how that force is applied.
Common causes include:
- assaults or interpersonal injury
- falls, particularly onto the chin
- sporting injuries
- motor vehicle or bicycle accidents
- high-impact trauma involving the face
A blow to the chin can transmit force through the lower jaw and sometimes affect the jaw joint, even if there is no obvious deformity at the point of impact.
The mechanism of injury matters because it can influence:
- where the fracture occurs
- whether more than one fracture is present
- whether other facial structures may also be involved, particularly the cheekbone or eye socket (orbit)
What Is a Broken Jaw?
A broken jaw is a fracture involving either the mandible, which is the lower jawbone, or the maxilla, which forms the upper jaw. In everyday language, “broken jaw” often refers to the lower jaw. In reality, the upper jaw can also fracture, and upper jaw injuries are often more closely related to broader midface trauma.
These injuries are not all the same.
A lower jaw fracture primarily affects how the jaw functions as a moving, tooth-bearing structure. This can disrupt bite alignment, chewing, speaking, and mouth opening, and may also affect sensation in the lower lip and chin.
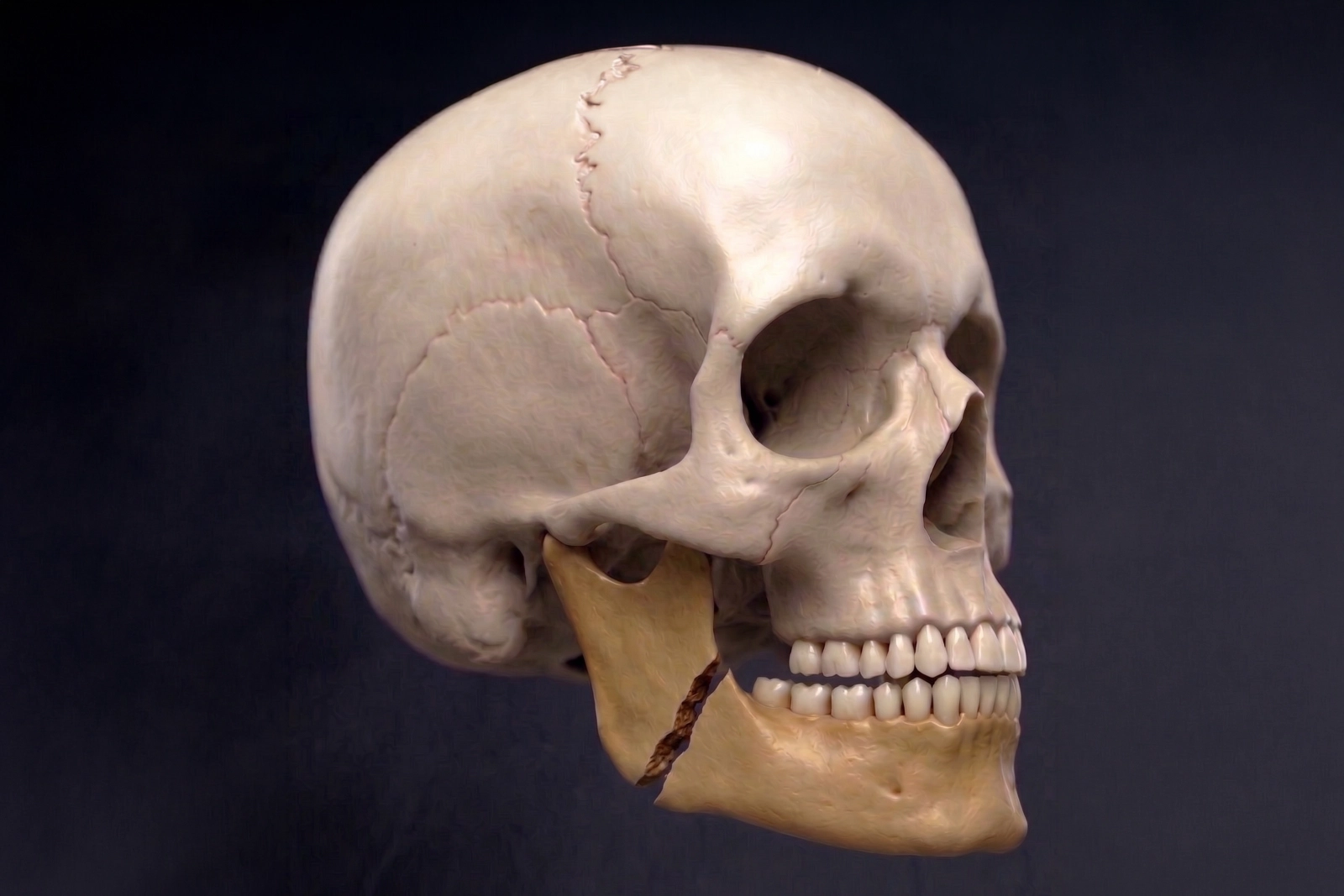
An upper jaw fracture affects the upper teeth and the middle part of the face (the “midface”), which includes the area around the nose, cheeks, and upper jaw. These injuries can change how the upper and lower teeth meet, affect facial support, and sometimes involve nearby structures such as the eye socket depending on the injury.
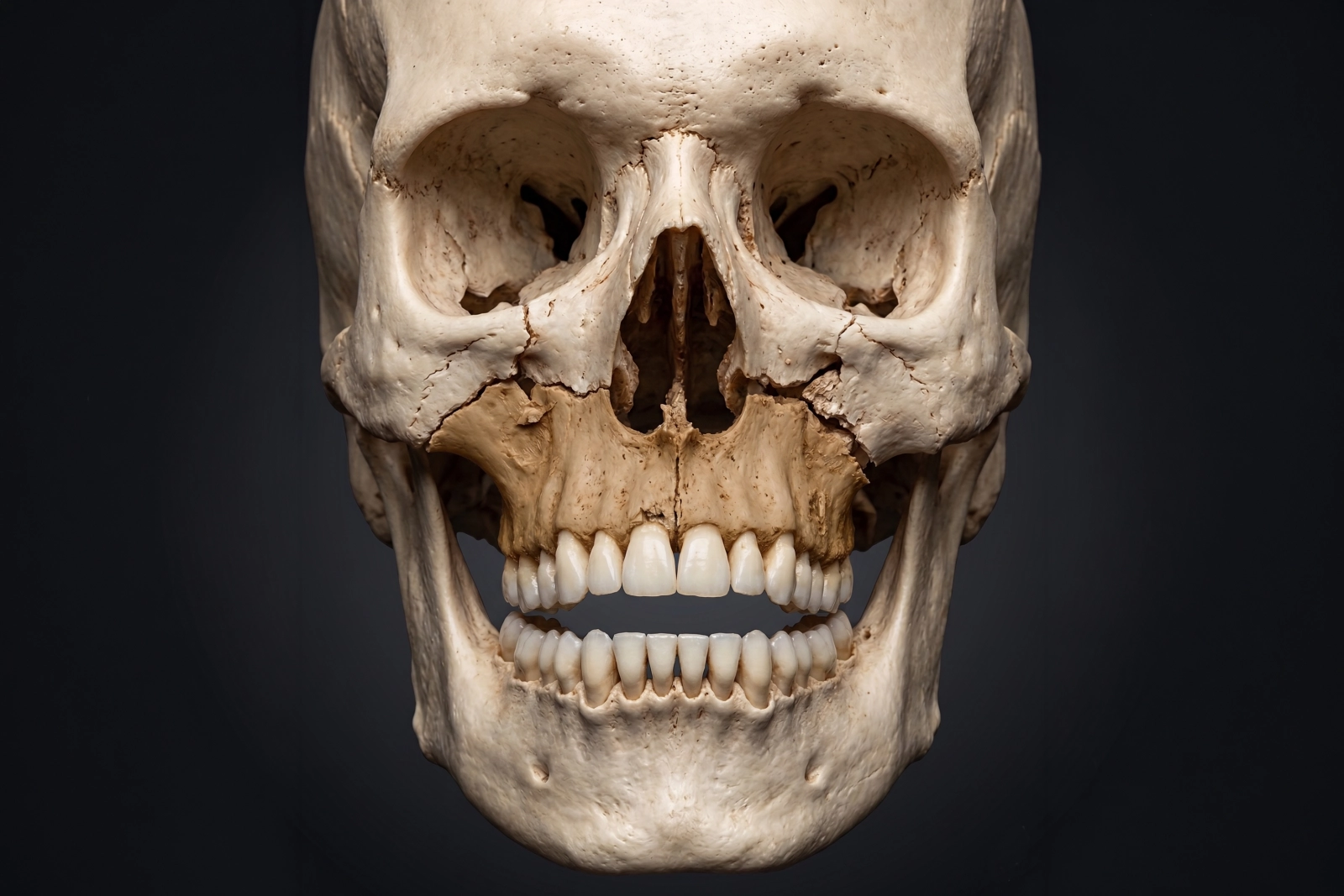
Why Bite Change Matters So Much
One of the biggest weaknesses in general discussions of jaw fractures is that they mention the bite but do not explain why it matters.
The jaw is not just a bone. It is part of a working system that has to bring the teeth together in a precise way for chewing, speaking, and normal function. When a fracture shifts the alignment of the jaw, even slightly, the change may be felt as:
- the teeth meeting unevenly
- only some teeth touching
- the jaw closing “crooked”
- the front teeth or back teeth no longer coming together properly
- a feeling that the bite is suddenly unfamiliar
That matters because a jaw fracture is not only about whether the bone is broken. It is about whether the jaw can heal in a position that restores a stable, comfortable, functional bite.
A new bite disturbance after trauma is one of the most important reasons a jaw injury should be assessed properly.
What Are the Symptoms of a Broken Jaw?
The symptoms depend on whether the injury involves the lower jaw or the upper jaw, and on whether the fracture is stable or displaced (bone ends have moved out of alignment).
Symptoms of a Lower Jaw (Mandible) Fracture
Lower jaw fractures are often dominated by bite and function.
Common symptoms include:
- a bite that feels different or “off”
- teeth that no longer line up properly
- pain with chewing
- pain when talking
- pain or restriction when opening the mouth
- swelling or bruising along the jawline
- tenderness over the jaw
- bleeding from the mouth or gum line
- loose teeth or a feeling that part of the tooth-bearing jaw moves
- numbness or tingling of the lower lip or chin
Some patients also notice pain near the jaw joint or below the ear, particularly if the injury involves the upper part of the mandible.
The lower jaw forms a ring-like structure. Because of this, a fracture in one area is often associated with a second fracture elsewhere in the jaw. This can make symptoms less straightforward, with pain in one area but changes in bite or function caused by a second, less obvious fracture.
Because these fractures often involve the teeth and mouth, there is also a risk of infection, which is why antibiotics are sometimes used in selected cases.
Symptoms of an Upper Jaw (Maxilla) Fracture
Upper jaw fractures are often under-recognised by patients because they may not immediately think of the upper jaw as part of a “broken jaw” problem.
Symptoms may include:
- a changed bite
- pain in the upper jaw or cheek area
- swelling and bruising in the middle part of the face
- discomfort when bringing the upper and lower teeth together
- a feeling that the upper jaw is loose or moving when it should not
- bleeding from the mouth or sometimes the nose depending on the injury
- difficulty chewing
- facial soreness after a higher-energy injury
Some upper jaw fractures are part of a broader injury pattern involving the midface, often alongside injuries such as cheekbone fractures, which affect the structure and contour of the face. The practical consequence for patients is that these injuries can affect both facial stability and bite.
Symptoms That Should Not Be Ignored
A jaw injury deserves careful assessment if you notice:
- a bite that has changed
- numbness of the lower lip or chin
- a mobile tooth-bearing segment
- upper jaw or midface movement
- bleeding from the mouth after trauma
- increasing pain with chewing or mouth opening
These features are more important than how dramatic the swelling looks.
How Is a Broken Jaw Diagnosed?
Diagnosis is based on both the mechanism of injury and a focused clinical examination. The goal is not simply to confirm a fracture, but to understand how it affects alignment and function.
A surgeon’s assessment focuses on how the injury occurred, whether the bite has changed, and how the jaw is functioning. Particular attention is paid to localised pain, restricted mouth opening, and whether any part of the jaw feels mobile or unstable.
The presence of bleeding inside the mouth, loose or misaligned teeth, or numbness affecting the lower lip or chin can provide additional clues about the location and severity of the injury.
These findings help determine not just whether a fracture is present, but how it is likely to behave and whether treatment may be required.
Examination Of the Bite
Checking the bite is one of the most important parts of the assessment.
If the upper and lower teeth no longer meet in the normal way, that raises concern that the jaw has fractured and shifted. A fracture can be present even if the face does not look dramatically abnormal from the outside.
Stability and Mobility
The assessment also looks at whether part of the lower jaw, upper jaw, or midface feels mobile. A mobile jaw segment is much more concerning than pain alone, because it suggests loss of stability and a greater chance that treatment will be needed to restore alignment.
Imaging
Imaging may include:
- X-rays, sometimes including a panoramic dental X-ray
- CT scanning when the injury is more complex, when plain imaging is not enough, or when the upper jaw or midface may be involved
The purpose of imaging is not only to confirm that a fracture exists. It is to understand:
- whether the fracture is displaced (bone ends have moved out of alignment)
- whether there is more than one fracture
- whether the tooth-bearing parts of the jaw are involved
- whether the upper jaw or midface is unstable
- whether surgical planning may be required
In other words, diagnosis is about pattern, position, and function, not simply yes-or-no confirmation of a break.
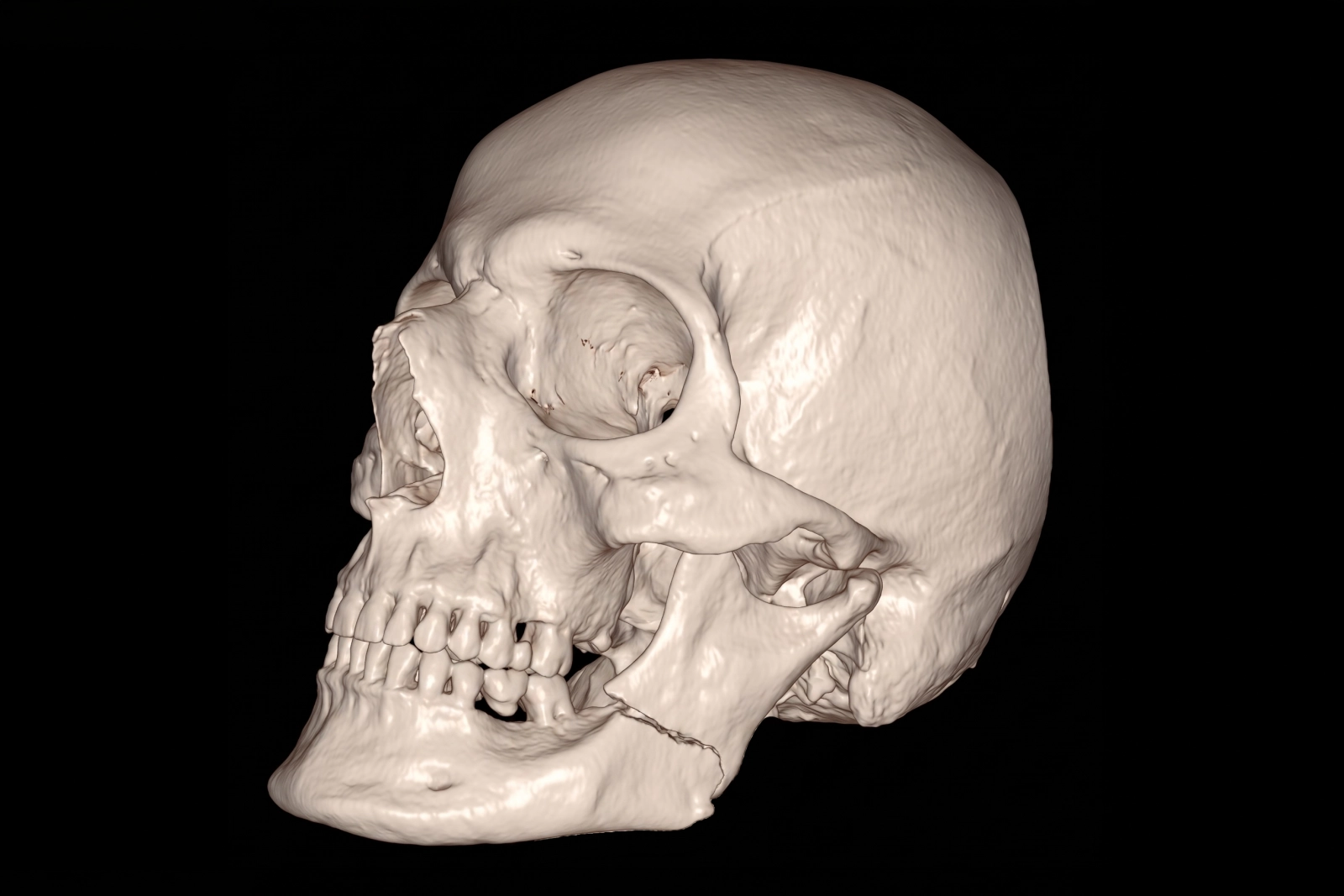
How Serious Is a Broken Jaw?
A broken jaw can range from a stable fracture with manageable symptoms to a more significant injury that affects bite, function, and facial stability.
A jaw fracture is more concerning when:
- the bite is disrupted
- part of the jaw is mobile or unstable
- the fracture is displaced
- the upper jaw or midface is involved
- there are multiple fracture sites
A fracture is considered displaced when the bone has shifted out of its normal position. A non-displaced fracture remains aligned. This distinction is important because displaced fractures are more likely to affect the bite and require intervention.
These features are important because they increase the likelihood that the jaw will not heal in acceptable alignment without intervention.
A fracture that looks less dramatic from the outside can still be clinically important if the bite is altered or the tooth-bearing jaw is unstable.
The key issue is not just whether the jaw is broken, but how much the injury affects function and alignment.
Does A Broken Jaw Always Need Surgery?
No. Not every jaw fracture needs surgery.
The key deciding factors are whether the bite is altered, whether the fracture is stable, and whether the bone has shifted out of position.
Lower Jaw (Mandible) Fractures
Some lower jaw fractures can be managed without surgery if they are:
- stable
- not significantly displaced (bone ends have not moved)
- associated with a normal bite
- not creating a mobile jaw segment
- not causing major functional difficulty
Surgery becomes more likely if:
- the bite is clearly altered
- the fracture is displaced
- part of the jaw is mobile
- there are multiple fracture sites
- the tooth-bearing segment is unstable
- chewing and jaw function are significantly affected
The key principle is that a lower jaw fracture is often judged less by the fact that a line is visible on imaging and more by whether the jaw remains aligned and functional.
Upper Jaw (Maxilla) Fractures
Upper jaw fractures are assessed differently because they may form part of a broader midface injury pattern.
Treatment becomes more likely if there is:
- mobility of the upper jaw
- instability of the midface
- disruption of the bite
- a fracture pattern unlikely to heal in a good position on its own
A minor, stable upper jaw injury is different from a more mobile upper jaw fracture. The more unstable the upper jaw is, the more likely treatment will be needed to restore the position of the jaw and the relationship of the teeth.
How Are Jaw Fractures Managed
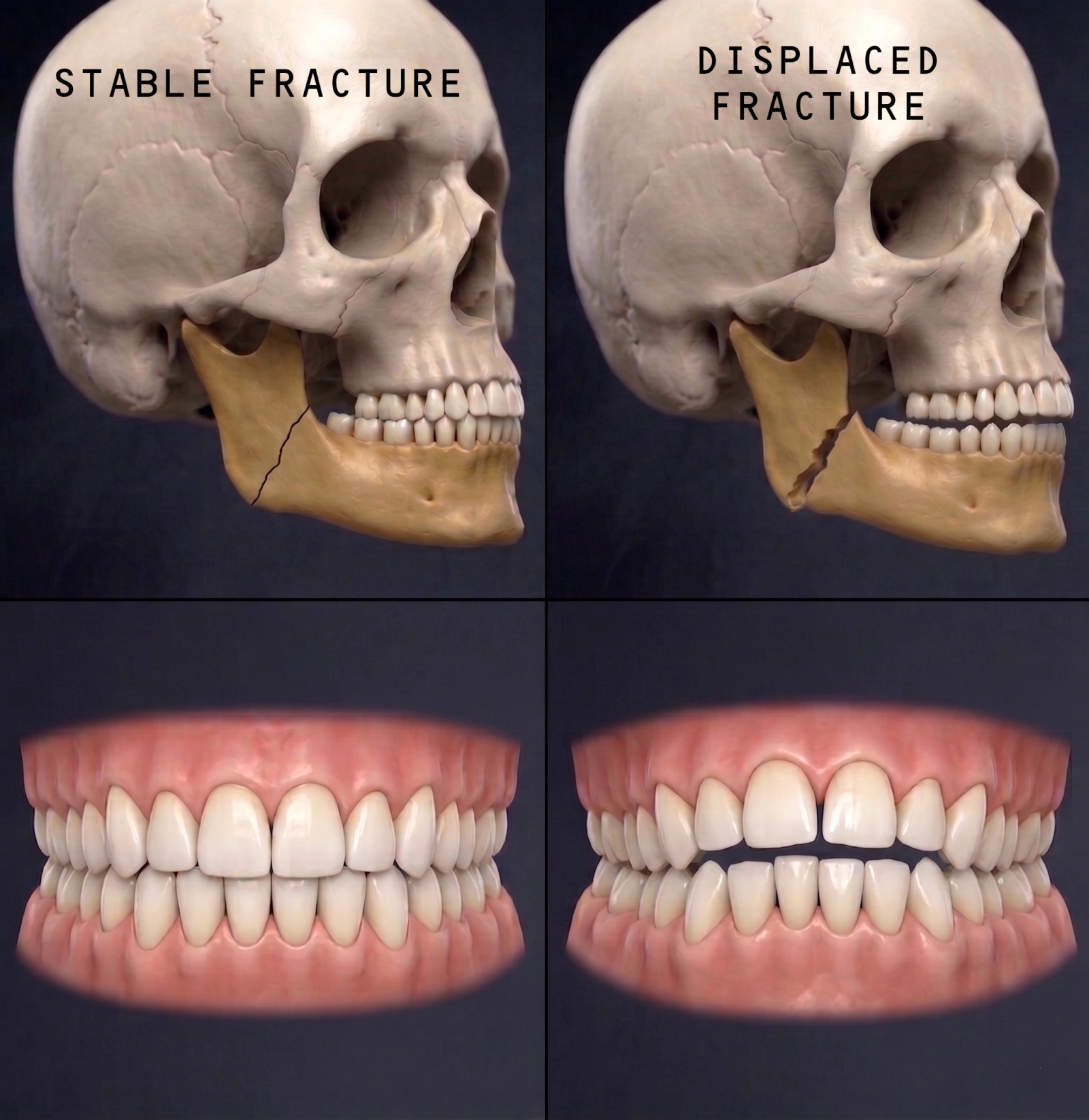
Treatment Pathway at a Glance
Treatment broadly follows one of two pathways, depending on whether the fracture is stable and whether the bite is affected.
Stable Pathway
This pathway is more likely when the fracture is stable, minimally displaced (bone ends have not moved), and does not significantly alter the bite or create a mobile segment.
Management typically involves a soft diet, pain relief, careful mouth care, and follow-up to ensure the bite remains stable as healing progresses.
Fixation (Surgery) Pathway
This is more likely when the fracture is displaced, unstable, or associated with a change in bite or function.
Management may involve reduction of the fracture (putting the bone back together in alignment) and stabilisation with plates and screws, along with measures to guide the bite during healing and review of alignment and function postoperatively.
This is a simplified way to understand the decision. The actual recommendation depends on the fracture pattern, examination findings, imaging, and overall injury context. This distinction between the stable and fixation pathways is central to decision-making: the question is not simply whether the bone is broken, but whether it can heal in a stable, functional position without intervention.
What Treatment Involves
Treatment depends on the fracture pattern, whether the lower jaw, upper jaw, or both are involved, and whether the injury has changed the bite or stability of the jaw.
Non-Surgical Treatment
Non-surgical treatment is usually appropriate when the fracture is stable and well aligned. This involves protecting the jaw while it heals, typically with a soft diet, avoidance of hard chewing, careful mouth care, and follow-up to monitor alignment and function.
Even when surgery is not required, the fracture still needs to be respected. The absence of an operation does not mean the injury is trivial. It still has to heal in the correct position.
Surgical Treatment
Surgery is used when the fracture needs to be realigned and stabilised so that the jaw can heal in the correct position. This is often done with plates and screws to hold the fracture segments while the bone heals. Further detail on how these injuries are assessed and treated is outlined on the facial trauma surgery page.
Surgical treatment is often performed through incisions inside the mouth, although the approach depends on the fracture pattern.
The aim of surgery is to restore:
- alignment
- bite
- stability
- function
For lower jaw fractures, that usually means restoring the relationship between the upper and lower teeth and stabilising the jaw so it heals without persistent malocclusion (bite feeling ‘off’).
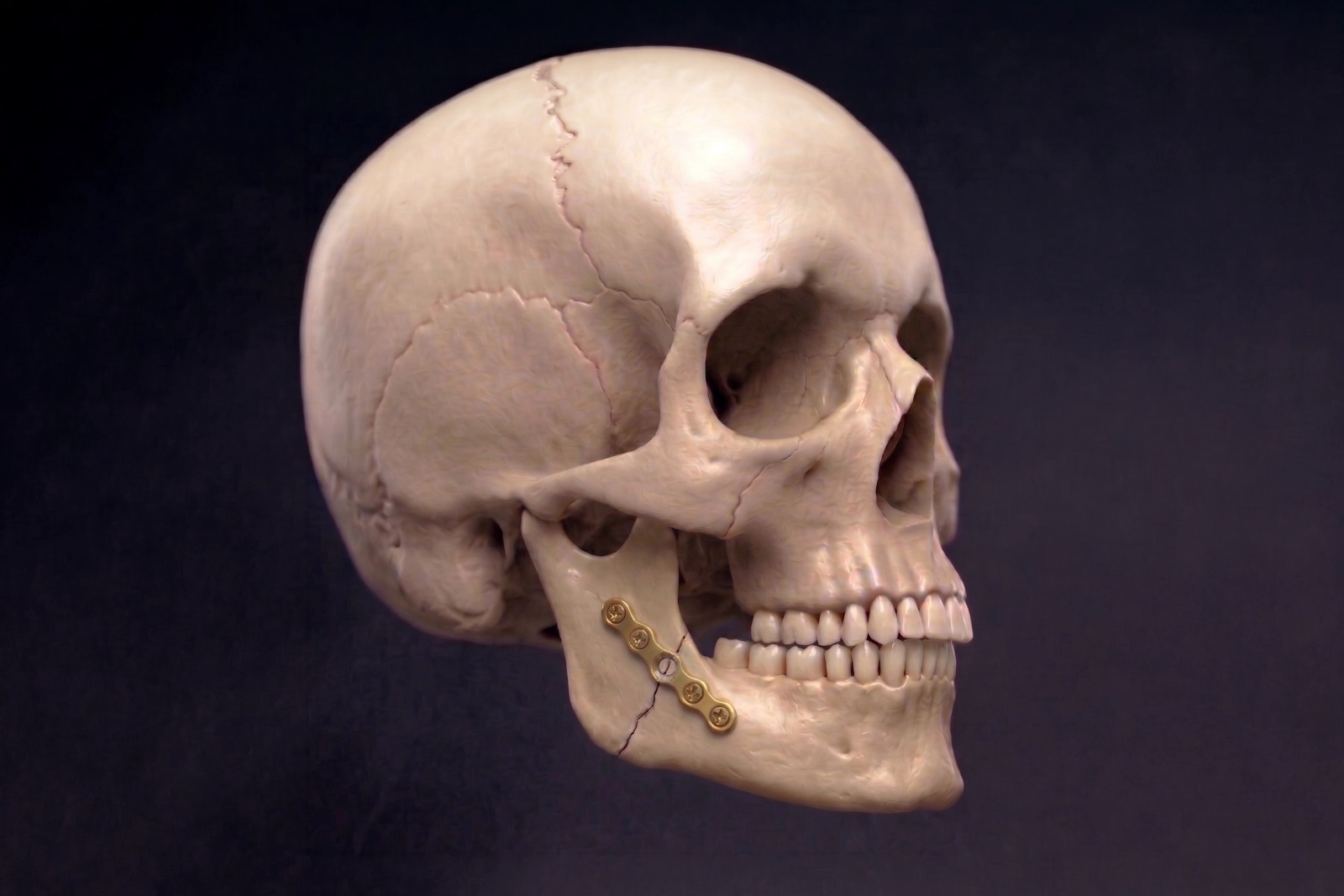
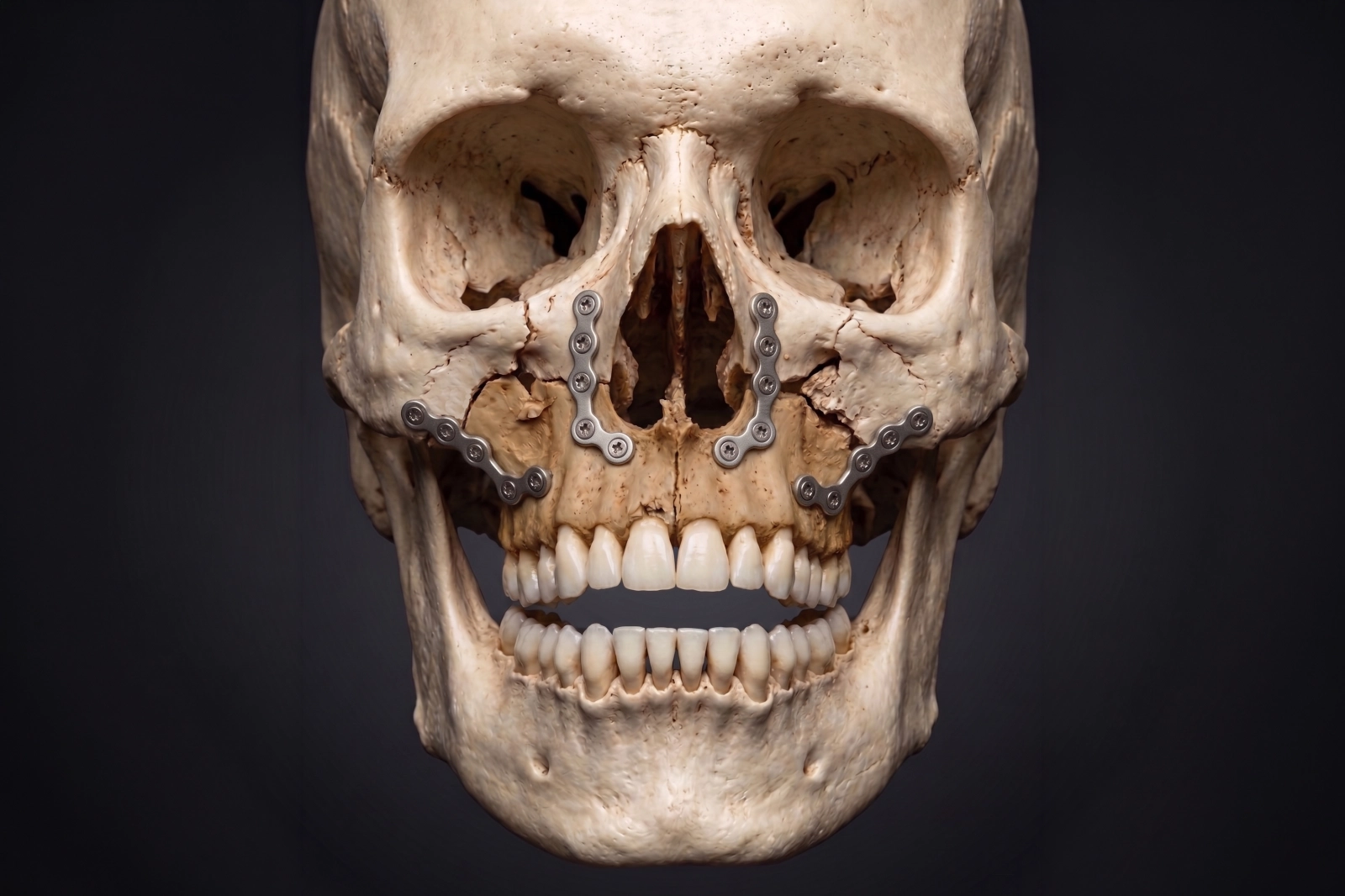
For upper jaw fractures, that may mean restoring the stability and position of the midface as well as the bite.
In more complex cases, treatment may involve reconstructive techniques similar to those used in jaw reconstruction after major tumour surgery.
Will My Jaw Be Wired Shut?
Most people think a broken jaw means the jaw will be wired shut. In many modern cases, this is not how treatment is performed.
Modern treatment more commonly involves internal fixation with plates and screws, sometimes with temporary elastics or other measures to guide the bite.
That does not mean wires or bite-guiding methods never have a role. They can still be used in selected situations. But the routine public image of prolonged jaw wiring does not reflect the way many fractures are managed now.
What Treatment Is Really Trying to Achieve
The goal is not just to show a fracture on a scan and “fix the bone.” It is to restore a jaw that is:
- stable
- aligned
- comfortable enough to function
- able to heal without leaving the bite disturbed
That is why treatment recommendations are centred on bite, mobility, stability, and function.
What Happens in Follow-Up
Follow-up is important whether treatment is surgical or non-surgical. It focuses on confirming that the bite remains acceptable, the fracture is healing in a stable position, and that mouth opening, pain, and swelling are improving over time.
It also allows monitoring of nerve symptoms such as numbness, and assessment of whether chewing function is gradually returning.
Follow-up matters because jaw fractures are dynamic injuries. Swelling can mask the true bite early, and a fracture that seemed acceptable at first may later show a clearer problem with alignment or function.
For patients, this means that review is not an optional extra. It is part of making sure the jaw heals in a way that restores long-term function.
Recovery After a Broken Jaw
Recovery depends on:
- which part of the jaw is fractured
- whether the fracture is stable or displaced
- whether surgery was required
- whether the bite was affected
- whether there are associated facial injuries
In the early stages, everyday activities such as eating, speaking, and cleaning the mouth may feel more difficult than expected. Over the following weeks, the focus is on protecting the healing jaw.
If the lower jaw nerve has been bruised, numbness of the lower lip or chin may persist and often improves gradually rather than immediately.
Healing Takes Time Even When Fixation Is Used
Plates and screws stabilise a fracture. They do not mean the bone is instantly healed.
Even after surgery, the jaw still needs time to consolidate. That is why diet and activity restrictions remain important for a period after fixation.
Recovery Is Not Just Bone Healing
A successful recovery is not only about the fracture line healing on imaging. It is also about:
- whether the bite feels right
- whether chewing becomes comfortable again
- whether mouth opening improves
- whether numbness settles
- whether the jaw feels stable and functional
An important part of recovery is confirming that the bite remains comfortable and aligned as swelling settles and healing progresses.
Recovery Timeline and Restrictions
- swelling, pain or tightness
- bruising
- modified diet and reduced chewing load
- improvement in comfort
- ongoing diet modification
- protection from further impact
- review of bite and function
- progressive return toward normal function
- reassessment of bite comfort
- cautious return to higher-risk activities only when healing is adequate
The exact timeline is not identical for every patient. A stable fracture managed without surgery is different from a displaced lower jaw fracture or a mobile upper jaw injury requiring fixation.
Eating, Speaking and Day-To-Day Function After a Jaw Fracture
One of the biggest burdens of a jaw fracture is that it affects basic daily function.
Eating
Chewing places force across the healing jaw, so food texture usually needs to be modified while healing is underway. The goal is to reduce stress on the fracture while still maintaining nutrition.
Speaking
Speaking is usually possible, but may be uncomfortable at first if there is swelling, stiffness, or pain with movement.
Mouth Care
Mouth care is especially important in jaw injuries because the fracture may involve the tooth-bearing jaw or wounds inside the mouth. Good mouth care supports comfort and local healing.
Daily Function
Jaw fractures are different from many other facial injuries because they interfere with:
- chewing
- speaking
- mouth opening
- bite comfort
- confidence using the jaw normally
That is why treatment decisions are so function-driven.
When Can You Return to Work, Gym or Sport?
Return to normal activity depends on the fracture pattern, treatment, and healing progress.
In general:
- desk-based work may resume sooner
- heavier physical work may need longer restriction
- contact sport or any activity with risk of another blow to the face usually needs the longest delay
Even if pain improves early, the healing jaw still needs protection. A second impact during healing can compromise the result.
Return to activity is usually guided by:
- fracture stability
- whether surgery was performed
- whether the bite is stable
- whether healing is progressing as expected
What Happens If a Jaw Fracture Is Left Untreated?
A jaw fracture that is stable and well aligned is not the same as one that is displaced or unstable. The main concern with leaving a clinically important fracture untreated is that it may heal in the wrong position.
Possible consequences include:
- persistent bite disturbance
- healing in poor alignment
- difficulty chewing
- ongoing discomfort or functional limitation
- persistent numbness
- instability
- delayed need for more complex correction
The most important long-term issue is often malocclusion. If the jaw heals with the bite out of alignment, that may be harder to correct later than it is at the time of the injury.
This is why a jaw injury should not be dismissed simply because swelling improves. If the bite feels different or the jaw feels unstable, proper assessment matters.
What Should You Do If You Think You Have a Broken Jaw?
If you think you may have a jaw fracture:
- seek medical assessment
- avoid chewing or placing force on the jaw
- protect the face from further impact
- do not ignore a change in your bite
Even if swelling improves, a change in bite or stability should be assessed to ensure the jaw heals correctly.
For a broader overview of how facial injuries are assessed and managed, including other types of fractures, see facial trauma and maxillofacial surgery.
Frequently Asked Questions
How do I know if my jaw is broken?
A broken jaw often causes a change in the bite, pain with chewing or opening the mouth, swelling, bleeding in the mouth, numbness of the lower lip or chin, or a feeling that part of the jaw is unstable after trauma. Diagnosis usually needs both examination and imaging.
What are the most important symptoms of a broken jaw?
The most important symptoms are often a changed bite, pain with movement, swelling, difficulty chewing, restricted mouth opening, numbness, or instability of the jaw after an injury.
Why does my bite feel different after injury?
A changed bite can happen when a fracture shifts the alignment of the upper or lower jaw. Even a subtle change matters because it may mean the jaw is no longer sitting in the correct position.
Can a broken jaw heal without surgery?
Yes, some stable and well-aligned fractures can heal without surgery. Fractures that are mobile, displaced, unstable, or associated with an altered bite are more likely to need fixation.
Will my jaw be wired shut?
Not necessarily. Many jaw fractures are now treated with plates and screws, sometimes with temporary elastics or bite-guiding measures rather than prolonged traditional wiring.
How long does a broken jaw take to heal?
Healing takes weeks, not days. Even when fixation is used, the bone still needs time to heal and the jaw often needs diet and activity restrictions during that period.
What can I eat with a broken jaw?
A modified diet is commonly needed while the jaw heals. This usually means avoiding hard or chewy foods and following a softer diet until healing is more advanced.
What is an upper jaw fracture?
An upper jaw fracture is a fracture of the maxilla. It may cause a changed bite, pain in the midface, and a feeling that the upper jaw or middle of the face is mobile or unstable.
Is a broken jaw an emergency?
It can be. Breathing difficulty, heavy bleeding, a clearly altered bite, major instability, or significant associated facial trauma all need urgent medical attention.
What happens if a jaw fracture is untreated?
A displaced or unstable fracture may heal in poor alignment, leading to bite problems, chewing difficulty, ongoing discomfort, numbness, or delayed corrective treatment.
Why is my lower lip or chin numb after a jaw injury?
Numbness of the lower lip or chin can occur when the nerve that runs through the lower jaw is affected by a fracture. This may be due to bruising or compression of the nerve. In many cases, sensation improves gradually over time, but recovery can vary depending on the injury.
About the Author
Dr Varun Harish is a Specialist Plastic, Reconstructive and Burns Surgeon (FRACS) with expertise in facial trauma and jaw reconstruction, including injuries affecting the mandible (lower jaw) and maxilla (upper jaw).
His practice includes the management of jaw fractures as well as reconstruction of the jaw following major trauma and cancer surgery, where precise restoration of bite, facial structure, and function is required.
He works within major Sydney hospital systems, including Royal North Shore Hospital and Liverpool Hospital, where complex facial injuries are managed as part of tertiary-level multidisciplinary care.
His clinical work focuses on restoring both function and facial contour, with careful assessment of when surgery is required and when it can be safely avoided. Dr Harish also makes use of advanced imaging and 3D planning techniques, including patient-specific modelling and 3D printing, to support accurate reconstruction of complex jaw defects.
He has also contributed to published research in facial trauma surgery, including work involving advanced intraoperative imaging to support accurate fracture reduction.
This combination of hospital-based trauma experience and reconstructive expertise informs a practical, patient-focused approach to facial fracture care, with an emphasis on restoring alignment, bite, and long-term function.
Dr Harish is the 2026 recipient of the Dr Ray Hollings Surgical Excellence Award (Northern Sydney Local Health District). He maintains an active academic and research interest in plastic and reconstructive surgery, with peer-reviewed publications and ongoing involvement in surgical education.
You can learn more about Dr Varun Harish here.
Educational information prepared by Dr Varun Harish FRACS, Specialist Plastic, Reconstructive & Burns Surgeon – Sydney.
Serving patients across the North Shore, Northern Beaches, Inner West and Central Coast.
Last reviewed April 2026.
Read how this site’s medical content is prepared and reviewed
