
Medicare for Tummy Tuck, Body Lift & Breast Reduction in Australia
Dr Varun Harish, FRACS Plastic Surgeon
First published:
Medicare for tummy tuck, body lift and breast reduction in Australia may apply in specific situations — but only when strict medical criteria under specific Medicare item numbers are met.
This guide explains the three most searched pathways: 30175 for post-pregnancy abdominal muscle separation with symptoms, 30179 for loose skin after major weight loss with skin and functional problems, and 45523 for heavy breasts causing physical symptoms (symptomatic macromastia).
Eligibility for Medicare rebates is determined based on clinical assessment and documentation against specific Medicare criteria. These criteria are designed to distinguish medically necessary procedures from purely cosmetic surgery (which is not covered by Medicare).
Does Medicare cover tummy tuck, body lift or breast reduction in Australia?
Medicare rebates for procedures such as tummy tuck, body lift, and breast reduction in Australia are only available when strict clinical criteria are met, including documented functional impairment and prior conservative management. These criteria are defined under specific Medicare Benefits Schedule (MBS) item numbers:
- 30175 for post-pregnancy rectus diastasis (separation of the abdominal “six-pack” muscles) with symptoms, which can occur following Caesarean section (C-section)
- 30179 for excess or loose skin after major weight loss with skin and functional problems, and
- 45523 for heavy breasts causing physical symptoms (symptomatic macromastia).
Even when criteria are met, there are usually out-of-pocket costs. In Sydney and NSW, these procedures are typically performed in the private hospital setting rather than as public hospital procedures.
Last reviewed: April 2026. This guide is based on the published wording of Medicare Benefits Schedule (MBS) items 30175, 30179 and 45523 at the time of review. Medicare item wording, explanatory notes, fees and benefits can change over time. This information aligns with the current MBS guidance and publicly available information from Services Australia.
 What “Medicare cover” means for tummy tuck, body lift and breast reduction
What “Medicare cover” means for tummy tuck, body lift and breast reduction
Medicare does not cover cosmetic surgery. It only provides a rebate for procedures that meet strict medical criteria.
Many people researching plastic surgery in Australia ask the same question: could Medicare apply, and what evidence would I need?
Many searches use terms like “Medicare tummy tuck Sydney,” “body lift covered by Medicare,” or “breast reduction Medicare,” but eligibility depends on whether a patient meets the criteria for a specific MBS item number. These criteria are strict and are based on the underlying problem, symptoms, prior treatment, and documentation, rather than how a procedure is described online. Terms like “C-section tummy tuck” are commonly used online, but Medicare eligibility depends on the underlying condition rather than the type of delivery.
This guide is designed to help readers understand how three commonly searched Medicare pathways work, what they do and do not mean, and what information is usually helpful before a specialist consultation. It also explains what these item numbers do not mean, what documentation may be helpful, and why eligibility cannot usually be determined from photographs alone.
This guide focuses on three commonly searched Medicare pathways in plastic surgery, but other item numbers may sometimes be relevant depending on the clinical problem and the operation being considered.
Which pathway might apply to you? A quick guide
These pathways are based on the underlying clinical problem, not the label used to describe the procedure.
In simple terms: 30175 relates to muscle separation after pregnancy, 30179 relates to excess or loose skin after weight loss, and 45523 relates to breast reduction for physical symptoms. A prior C-section may be part of the history for 30175, but Medicare criteria relate to muscle separation after pregnancy rather than the C-section itself.
 Medicare for Tummy Tuck, Body Lift & Breast Reduction: At a glance
Medicare for Tummy Tuck, Body Lift & Breast Reduction: At a glance
Medicare may apply in some medically indicated situations.
- 30175 is for a pregnancy-related problem, with imaging (such as ultrasound or CT scans) showing separation of the abdominal six-pack muscles (rectus diastasis) of at least 3 cm, documented symptoms that affect comfort or activity, failed treatment including physiotherapy, and no pregnancy in the last 12 months. It is listed as applicable once per lifetime. A prior C-section may be part of the history, but Medicare criteria relate to muscle separation after pregnancy rather than the C-section itself.
- 30179 is for circumferential (all the way around the trunk in a 360° pattern) lipectomy (skin removal) after significant weight loss where the excess or loose skin and tissue is causing rashes or irritation between skin folds (intertrigo), has failed at least 3 months of conventional treatment, interferes with daily activities, and weight has been stable for at least 6 months after significant weight loss. MBS explanatory notes define significant weight loss for relevant lipectomy items as at least 5 BMI units.
- 45523 is for breast reduction (bilateral reduction mammaplasty with surgical repositioning of the nipple) in patients with macromastia (heavy breasts), who are experiencing pain in the neck or shoulder region.
In practice, many people who search for these procedures do not meet the strict Medicare criteria, even though their concerns are real and important. Medicare item applicability is assessed against strict published criteria and is subject to audit.
When Medicare usually does NOT apply
- When the concern is primarily appearance rather than a medical problem
- When required symptoms are not documented
- When imaging or diagnostic criteria are not met
- When conservative treatment has not been tried
- When weight is not yet stable after weight loss
What Medicare does and does not mean
What Medicare may mean
A Medicare item number does not mean surgery is free. It means there may be a rebate toward part of the surgical fee if the relevant criteria are met and the procedure performed is the appropriate one.
What Medicare does not mean
Out-of-pocket costs, hospital arrangements, health fund considerations, anaesthetic fees, and other practical issues are separate considerations. Even when people refer to a procedure as being “covered by Medicare,” this usually means a partial rebate rather than full cost coverage for treatment. This means that there are usually costs over and above the Medicare rebate. Some patients also choose to proceed outside Medicare criteria as self-funded patients when their concerns are not covered by a specific item.
What does this mean for cost in practice?
In practical terms, when people ask about “Medicare cover” for procedures like tummy tuck, body lift, or breast reduction, they are usually asking how much they will need to pay.
If a Medicare item applies, there may be a rebate toward part of the surgical fee. However:
- there are usually additional costs for hospital care, anaesthesia, and other components of treatment
- private health insurance may cover some hospital costs depending on your policy
- there are typically out-of-pocket costs even when Medicare criteria are met
The exact cost varies depending on the procedure, clinical situation, and hospital setting. A consultation is usually required to provide an accurate estimate.
How private health insurance interacts with Medicare
Private health insurance may cover some hospital costs when a Medicare item applies, depending on your level of cover. This typically relates to:
- Hospital accommodation
- Theatre fees
It does not usually cover the full surgeon’s or anaesthetist’s fees. Patients without appropriate hospital cover may still proceed, but hospital costs are then self-funded.
Understanding your level of cover is an important part of planning.
Practical implications in Sydney, NSW
Tummy tuck, body lift and breast reduction procedures are not performed as Medicare-patient procedures in NSW public hospitals. In practice, in Sydney and NSW, where surgery is considered under these item numbers, it is typically performed in a private hospital.
How much does surgery cost with Medicare in Australia?
In Australia, when a Medicare item number applies, Medicare provides a rebate toward part of the surgical fee. This does not mean the procedure is fully covered.
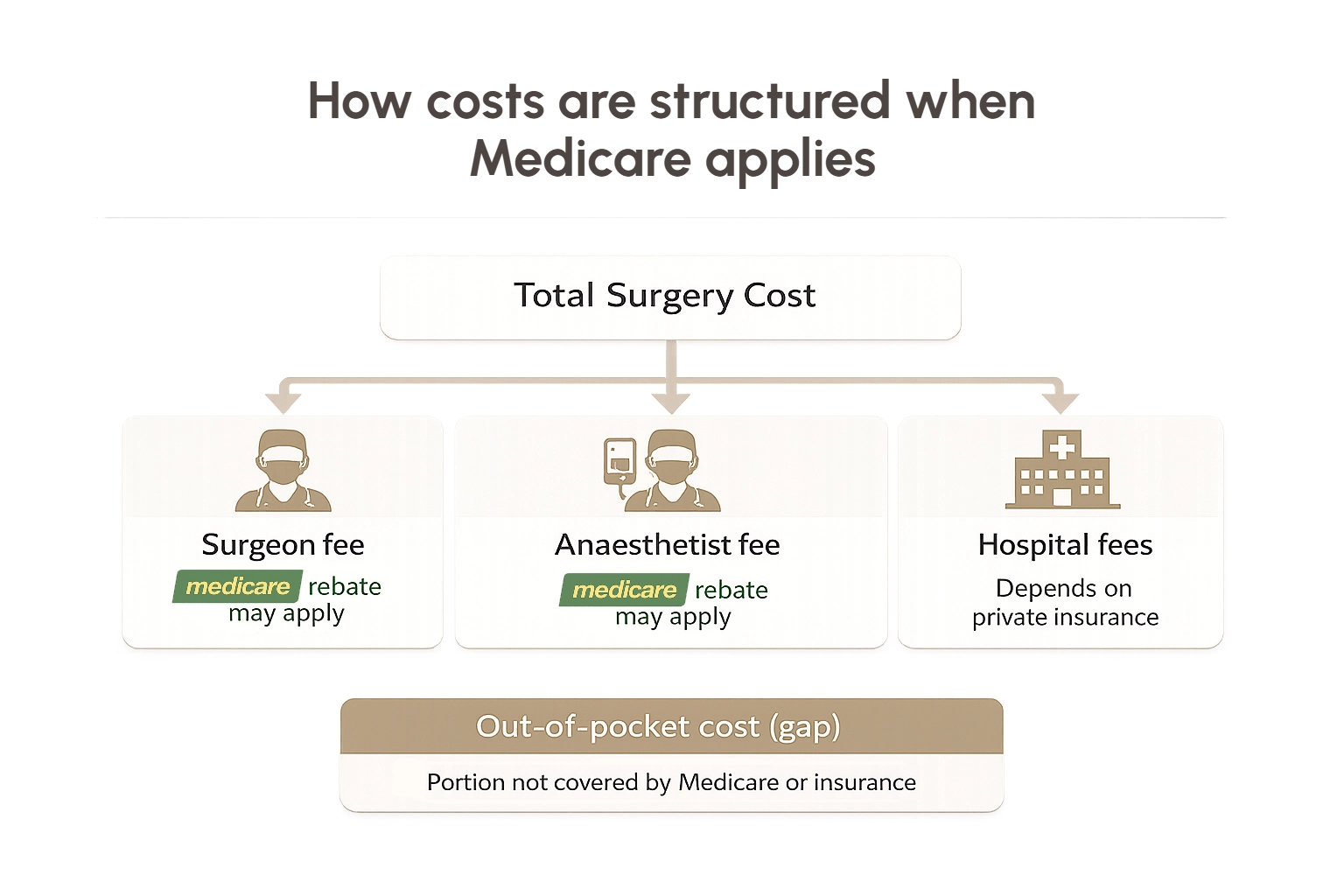
In practical terms, total costs are usually made up of several components:
- Surgeon’s fee (partially rebated if Medicare criteria are met)
- Anaesthetist’s fee (partially rebated if Medicare criteria are met)
- Hospital fees or private health fund excess
Typical out-of-pocket costs vary depending on the procedure, complexity, and hospital setting. As a general guide:
- Procedures such as tummy tuck (including 30175) or body lift (30179) often involve significant out-of-pocket costs even when Medicare applies
- Breast reduction (45523) may have lower out-of-pocket costs compared to abdominal procedures, but is still not fully covered
Private health insurance may cover some hospital costs depending on your level of cover, but does not eliminate out-of-pocket expenses.
Because of these variables, an individualised estimate is usually only possible after consultation.
Formal assessment still matters
It is also important to separate meeting criteria for Medicare from being suitable for surgery. These are related, but not identical. A person can have concerns that are real and important without meeting Medicare item criteria. The opposite is also true – meeting the relevant Medicare item number criteria does not replace proper assessment, discussion of options, timing, recovery, risks, or whether surgery is actually the right next step.
Online information can help you understand the framework, but it cannot confirm Medicare item applicability in an individual case. Formal assessment depends on the exact clinical problem, documentation, examination, and where relevant, imaging.
Quick Medicare snapshot
| Medicare item number | Typical scenario | What usually needs to be true | Common reasons it may not apply |
|---|---|---|---|
| 30175 | Pregnancy-related abdominal wall problem (rectus diastasis), sometimes following a C-section | - Imaging-confirmed muscle separation ≥3 cm - Symptoms affecting function (e.g. discomfort, weakness, back pain, urinary symptoms) - Failed physiotherapy or non-surgical treatment - No pregnancy in the last 12 months - A C-section may be part of the history but is not the qualifying factor | - If the main concern is loose skin only - No symptoms - No imaging - No trial of conservative treatment - Recent pregnancy |
| 30179 | Circumferential loose or excess skin after weight loss | - Circumferential (all the way around – 360°) excess following significant weight loss - Rashes or another skin condition related to loose skin - Failed ≥3 months of treatment - Interference with daily activities - Weight stable ≥6 months after significant weight loss | - Excess skin is not circumferential - No documented skin condition - No failed treatment history - Weight not yet stable - Concern is primarily appearance |
| 45523 | Breast reduction | - Macromastia (heavy breasts) causing neck or shoulder pain - Symptoms documented (e.g. discomfort, posture-related strain, bra strap grooving) - Appropriate breast reduction procedure planned - Not for cosmetic enlargement or implant-based procedures | - No symptoms - Medicare item is confused with cosmetic breast surgery |
This is the short version only. Whether a particular item applies still depends on the full clinical picture and the operation being proposed.

If you think your situation may meet Medicare criteria, the next step is a formal assessment.
This usually involves reviewing your symptoms, prior treatment, and any imaging, and determining whether your clinical situation aligns with a specific MBS item.
You can request a referral from your GP or arrange a consultation to assess your individual circumstances.
Common scenarios people mix up
C-section shelf vs rectus diastasis
A C-section shelf, pouch, lower abdominal bulge, or postpartum tummy bulge may reflect scar tethering, skin excess, fat distribution, rectus diastasis, or separation of the abdominal muscles, or a combination. A visible lower abdominal pouch is not the same thing as a Medicare-eligible pregnancy-related problem in the abdominal muscles. A C-section may be part of the history but is not the qualifying factor. For more information about C-section shelf or bulge after C-section, read our guide.
Lower abdominal overhang vs circumferential excess
A lower abdominal apron, pannus, apron after weight loss, or overhang does not automatically mean the excess is circumferential or all the way around. The Medicare number 30179 is aimed at excess skin and tissue extending around the trunk in a belt-like pattern, with skin and functional consequences after significant weight loss. For more information about loose or excess skin after weight loss, read our guide.
Large breasts vs symptomatic macromastia
Breast size alone does not determine eligibility. The relevant issue is whether breast weight is causing documented physical symptoms such as neck or shoulder pain.
Quick comparison guide
| What someone notices | What it may reflect | Does it automatically map to a Medicare item? |
|---|---|---|
| C-section shelf, pouch or bulge | Scar tethering, skin excess, fat distribution, split abdominal muscles, or a combination | No. 30175 only applies if the formal pregnancy-related muscle-separation criteria are met. |
| Lower abdominal overhang or apron after weight loss | Localised lower abdominal excess or broader circumferential excess around the trunk | No. 30179 is aimed at circumferential excess with skin and functional consequences, not every lower abdominal overhang. |
| Large or heavy breasts | Breast size alone, or symptomatic macromastia with documented physical symptoms | No. 45523 depends on the symptom pattern, and proposed operation. |
Some patients do not fit neatly into a single Medicare pathway
In practice, some patients have a combination of concerns, such as abdominal muscle separation (rectus diastasis) together with excess skin, or weight-loss changes that are not fully circumferential. In these situations, the most appropriate item number, if any, depends on the dominant clinical problem, the findings on assessment, and the operation being performed.
Example scenarios (how this applies in practice)
- A patient after pregnancy and C-section with a visible lower abdominal bulge or pouch but no documented muscle separation may not meet criteria for 30175.
- A patient after significant weight loss with excess skin mainly at the front, but not extending around the trunk and without skin problems, may not meet criteria for 30179.

If you're unsure which pathway your situation falls into, a structured assessment is usually more helpful than trying to match symptoms to item numbers alone.
Tummy tuck after pregnancy (Medicare item 30175)
Who may qualify for 30175?
Medicare item 30175 is a rebate for tummy tuck after pregnancy only when there is a confirmed rectus diastasis (separation of the 'six-pack’ abdominal muscles) of at least 3 cm, documented symptoms, and failed non-surgical treatment.
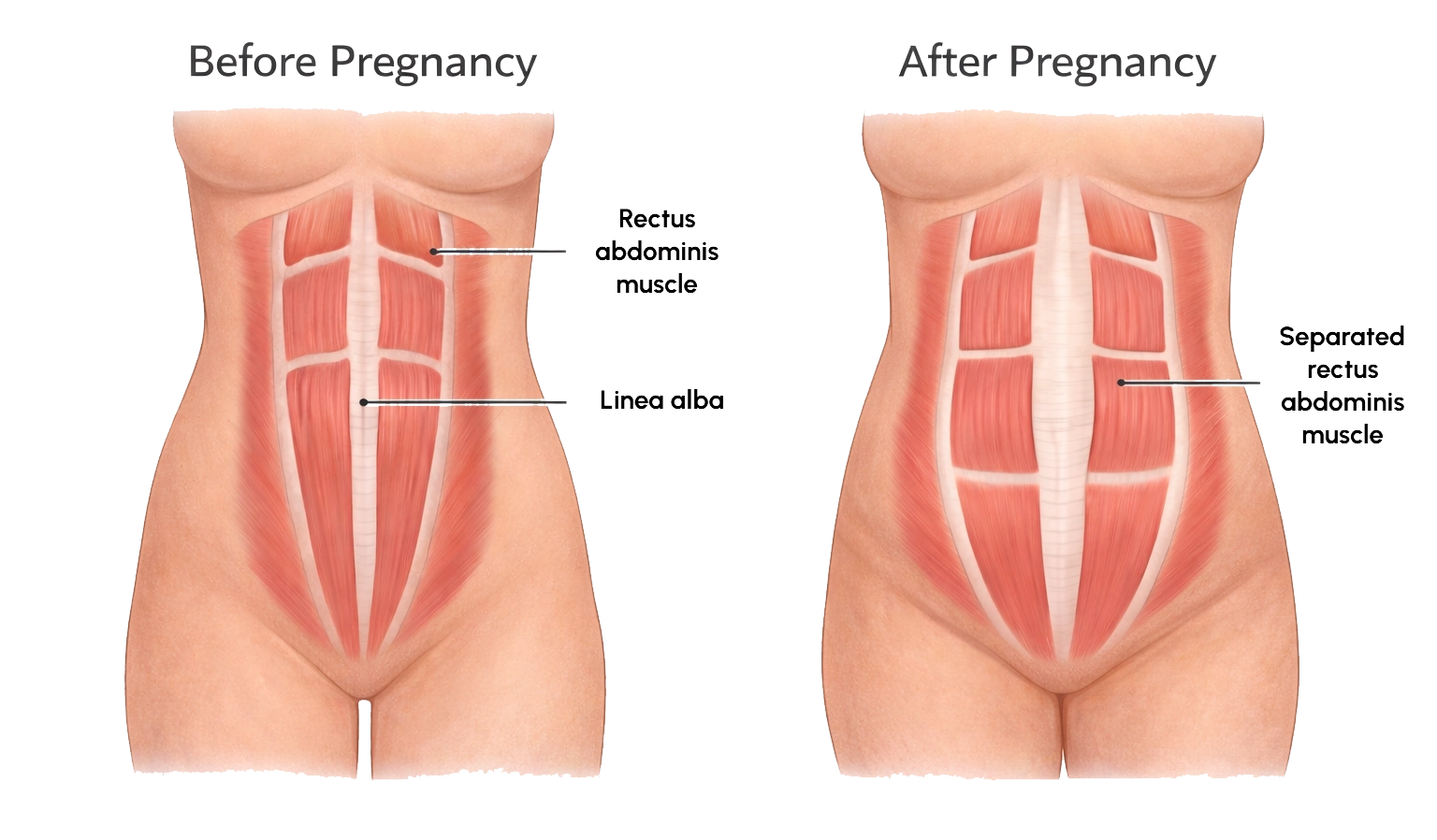
What 30175 is intended for
This item is often misunderstood. It is not a blanket “Medicare tummy tuck” item. It is a specific Medicare item for radical abdominoplasty (tummy tuck) with repair of muscle separation (rectus diastasis) in a patient who has a pregnancy-related structural problem in the abdominal muscles and meets all listed criteria. A visible contour concern is not the same thing as a qualifying problem in the abdominal muscles that causes symptoms.
A prior C-section may be part of the history, but it is not the qualifying factor — the relevant issue is pregnancy-related muscle separation with symptoms.
What does this mean in practice?
Medicare item 30175 refers to pregnancy-related separation of the six-pack abdominal muscles (rectus diastasis) that causes symptoms and meets strict clinical criteria.
The symptoms of abdominal wall weakness (or post-pregnancy muscle separation, split abdominal muscles, core weakness after pregnancy), include discomfort with activity, low back pain, or urinary symptoms.
This pathway is generally considered once recovery from pregnancy is complete and symptoms have persisted despite non-surgical treatment.
In simple terms, this pathway applies when muscle separation after pregnancy is causing symptoms and has not improved with non-surgical treatment. Many patients associate this with a C-section, but Medicare criteria are based on the underlying rectus diastasis rather than the presence of a C-section scar.
What are the Medicare requirements?
Under Medicare rules, the patient must have:
- rectus diastasis (split abdominal muscles) of at least 3 cm measured by scans
- symptoms of pain or discomfort during functional use, and/or low back pain or urinary symptoms
- failure to respond to non-surgical conservative treatment including physiotherapy
- no pregnancy in the last 12 months
What documentation may help for 30175
Helpful records often include:
- a GP summary of symptoms and timeline
- an imaging report (e.g., ultrasound or CT scan) documenting muscle separation
- notes about pain, abdominal wall weakness, functional difficulty, low back symptoms, or urinary symptoms
- evidence of a course of conservative treatment, especially physiotherapy
Acceptable examples of conservative non-surgical treatment must include physiotherapy, and may also include pain medication, braces, lifestyle changes, and exercise.
Common reasons 30175 may not apply
- the main issue is contour, fullness, or a visible lower abdominal pouch without a qualifying pregnancy-related problem in the abdominal muscles
- there is no imaging showing diastasis of at least 3 cm
- symptoms do not include core weakness or pain
- conservative treatment, including physiotherapy, has not yet been tried
- pregnancy was within the last 12 months
Body lift after weight loss (Medicare item 30179)
Who may qualify for 30179?
Medicare item 30179 is a rebate for body lift after weight loss when excess skin is circumferential (all the way around the trunk in a 360-degree pattern) and causes documented skin problems and functional limitation after stable weight loss.
What 30179 is intended for
Medicare item 30179 is the key Medicare item for patients searching terms like body lift Medicare, circumferential lipectomy Medicare, belt lipectomy Medicare, or Medicare after massive weight loss. It applies to 360° belt lipectomy or body lift surgery as an independent procedure to correct excess skin that is all the way around and is a direct consequence of significant weight loss. Loose lower abdominal skin (not all the way around) is not the same as circumferential excess around the trunk.
What does this mean in practice?
Medicare item 30179 is for circumferential (all the way around) excess skin after significant weight loss when it causes skin problems and functional limitation.
The important word here is circumferential. This is not simply loose lower abdominal skin or an isolated apron at the front. It describes loose skin that wraps around the trunk like a belt, affecting the abdomen, flanks, waistline, and lower back in a 360-degree pattern. That is why this item is most relevant to body lift rather than a straightforward tummy tuck discussion.
In practice, this pathway is considered once weight has been stable for several months and ongoing skin problems or functional limitations are clearly established.
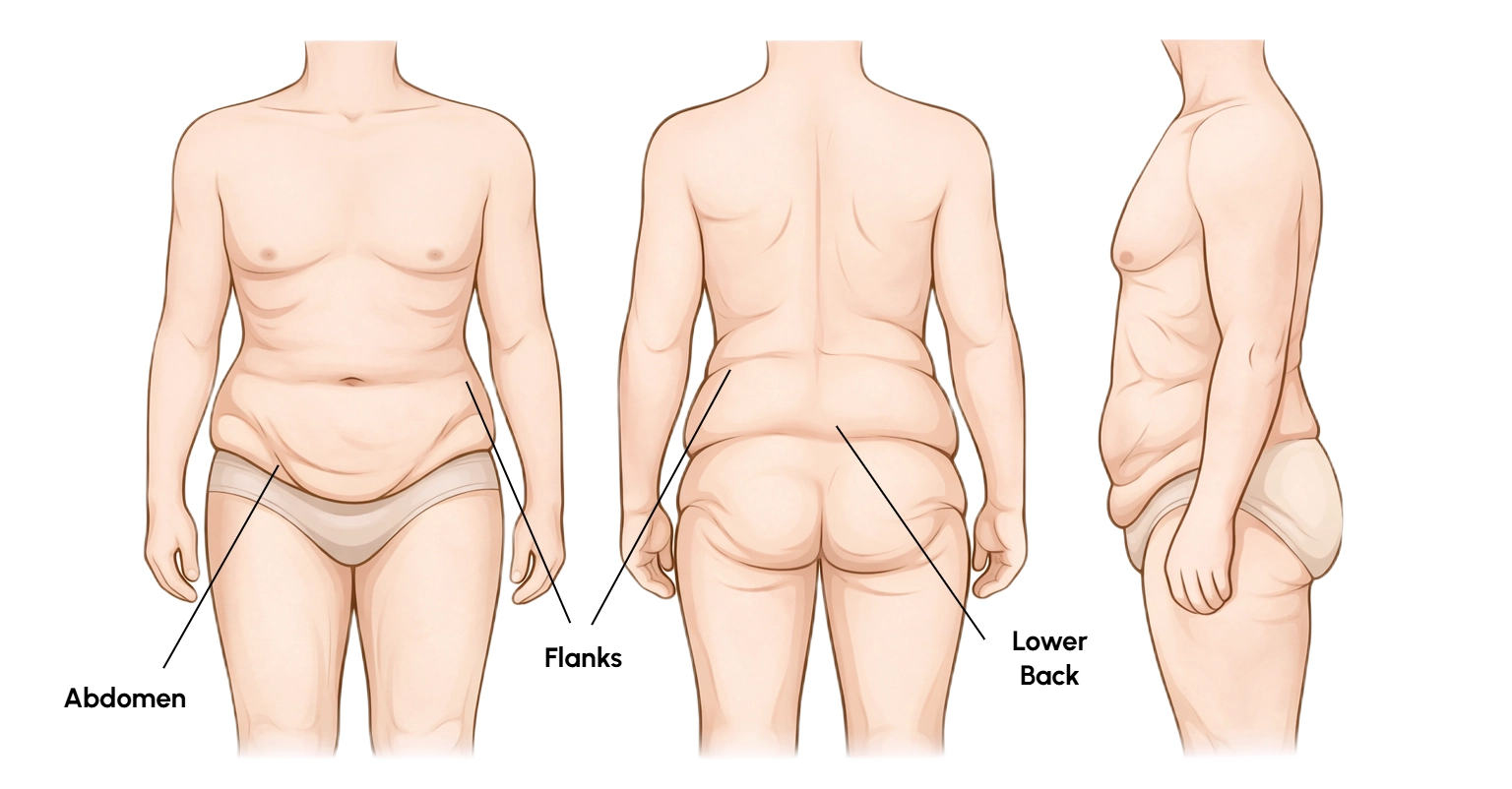
What are the Medicare requirements?
For 30179, Medicare requires:
- circumferential excess of redundant skin and fat complicated by intertrigo or another skin condition that risks loss of skin integrity
- failure of 3 months of conventional or non-surgical treatment
- interference with activities of daily living
- weight stable for at least 6 months after significant weight loss
What “significant weight loss” means
Medicare defines significant weight loss for items as a reduction equivalent to at least 5 BMI units, with weight stable for at least six months before surgery.
What documentation may help for 30179
Helpful records often include:
- GP notes describing recurrent intertrigo, skin irritation, skin fold rash, or skin breakdown risk
- documentation of conventional treatment tried over at least 3 months
- weight history showing significant weight loss and later stability
- relevant records from dermatology, wound care, or other treating clinicians if involved
This does not mean patients should try to “collect evidence” to fit an item. It simply means that when a condition has genuinely been causing ongoing problems, accurate documentation becomes important.
A useful distinction: 30179 is not the same as every weight-loss tummy tuck
Some people after significant weight loss have a lower abdominal apron or pannus without true circumferential excess. Others have a much broader 360-degree pattern affecting the whole lower trunk. Some may also come across 30177, another related Medicare item number associated with redundant abdominal skin and fat after significant weight loss in conjunction with radical abdominoplasty. This guide focuses on 30179 because it is the clearest body-lift-style circumferential pathway, but not every post-weight-loss abdomen fits the same Medicare item.
Common reasons 30179 may not apply
- excess tissue is mainly at the front rather than circumferential
- there is no documented skin condition
- conventional treatment has not been tried for at least 3 months
- weight is still changing
- the main concern is appearance rather than skin integrity/quality or functional impact
Breast reduction Medicare (Medicare item 45523)
Who may qualify for 45523?
Medicare item 45523 is a rebate for breast reduction surgery in patients with macromastia (heavy breasts) causing neck or shoulder pain.
What 45523 is intended for
Medicare item 45523 is the main Medicare item patients usually mean when they search Medicare breast reduction. The current item wording is for bilateral reduction mammaplasty with surgical repositioning of the nipple for patients with macromastia who are experiencing pain in the neck or shoulder region, and not with insertion of any prosthesis. In practical terms, this refers to a formal breast reduction procedure that reduces breast weight and repositions the nipple (lifts it higher). The Medicare item also applies to a specific type of breast reduction operation, not all techniques or variations.
Having large breasts alone does not automatically qualify under the item wording. Procedures that increase breast size, such as breast augmentation with implants, do not meet Medicare criteria.
What does this mean in practice?
Medicare item 45523 is for breast reduction in patients with large or heavy breasts causing physical symptoms such as neck or shoulder pain.
In plain language, this pathway is about heavy breasts causing physical symptoms, not just breast size or appearance. Some patients may also describe associated features such as bra strap grooving, upper back discomfort, posture-related strain, or recurrent irritation, but the MBS descriptor itself centres on macromastia with pain in the neck or shoulder region. The question is not simply breast size, but whether the clinical problem and proposed operation for breast reduction meet Medicare’s criteria. Procedures that increase breast size, such as breast augmentation with implants, do not meet Medicare criteria.
Common mistakes people make with 45523
The first is assuming that all breast reduction surgery is automatically covered. It is not. The item is tied to a specific operation type and a specific symptom framework.
The second is assuming that Medicare eligibility is determined by a single online rule such as cup size or an internet forum’s “grams removed” threshold. Medicare rules apply to symptoms and the type of breast reduction procedure being performed, rather than listing a minimum amount of tissue to be removed.
What documentation may help for 45523
Helpful information may include:
- GP documentation of neck or shoulder pain
- notes about bra strap grooving, activity limitation, posture-related symptoms, upper back discomfort, or recurrent skin irritation if relevant
- records of non-surgical management already tried
- allied health history where relevant, such as physiotherapy
The important point is not to inflate symptoms, but to make sure the medical record accurately reflects the problem the patient is actually living with.
Common reasons 45523 may not apply
- the issue is framed only as breast size or appearance without documented symptoms
- the proposed procedure for breast reduction is different to Medicare’s criteria
- neck or shoulder pain and related functional symptoms are not clearly documented
Decision summary table
| Scenario | Medicare likely? |
|---|---|
| Cosmetic concern only | No |
| Functional symptoms (e.g. rashes, back pain) | Possible |
| Meets strict MBS criteria | Yes |
| Documentation incomplete | No |
Common misconceptions
Many patients assume Medicare will cover procedures like tummy tuck or breast reduction automatically, but eligibility depends on specific clinical criteria rather than the procedure itself.
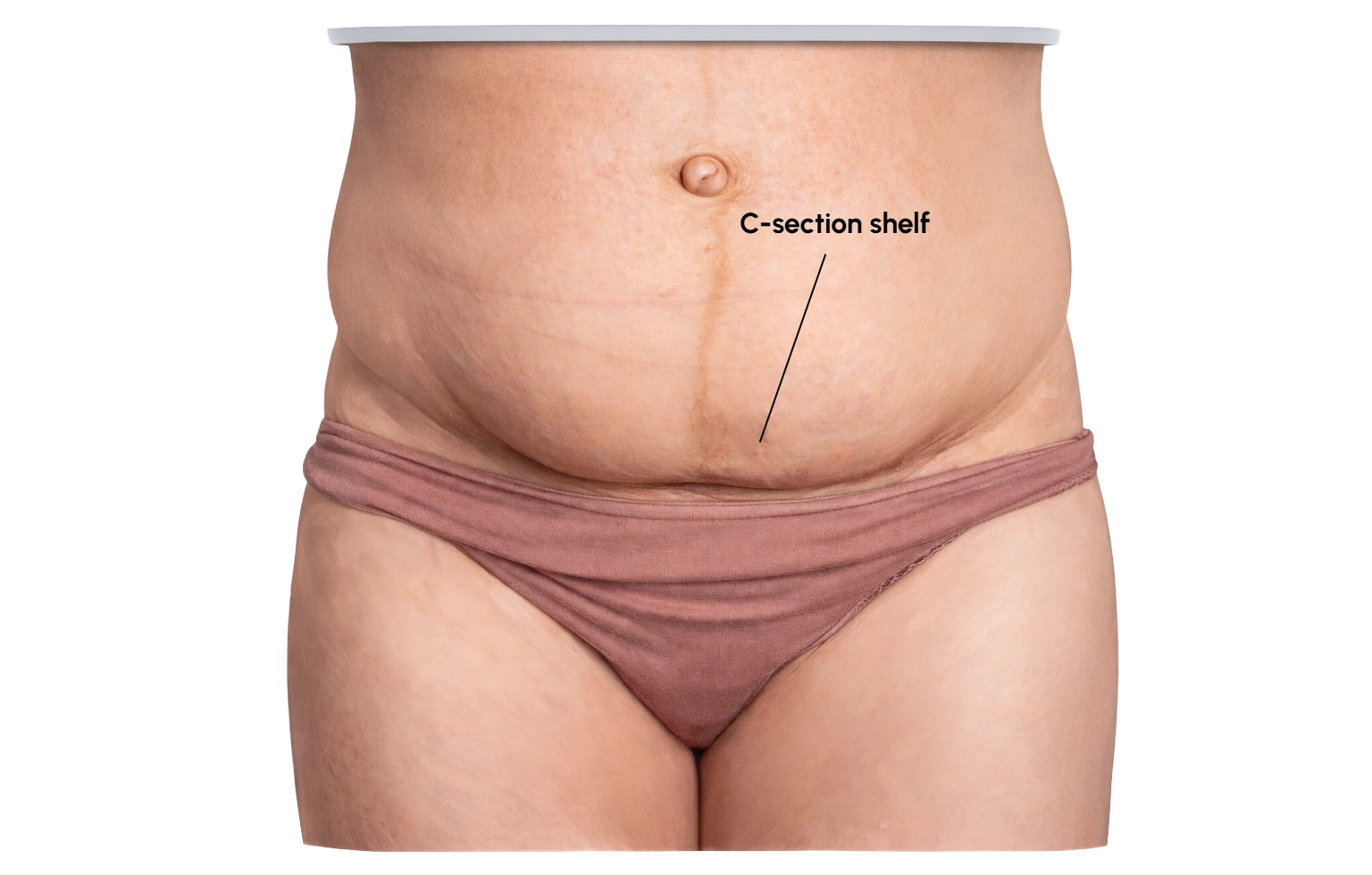
“If I have a C-section shelf, Medicare covers tummy tuck.”
Not necessarily. A visible shelf, pouch, or lower abdominal bulge can reflect scar tethering, skin excess, fat distribution, muscle separation, or a combination of factors. Medicare applies in certain scenarios as outlined above. A visible change is not automatically the same as meeting Medicare criteria.
“If I have lost a lot of weight, I automatically qualify for a body lift rebate.”
No. Medicare item 30179 requires more than weight loss alone. It requires belt-like or 360° loose skin after significant weight loss, a skin condition, failed previous treatment, interference with daily living, and stable weight for at least 6 months.
“Breast reduction is always covered by Medicare.”
No. Medicare item 45523 is tied to a patients with heavy breasts experiencing pain in the neck or shoulder region and the technique of breast reduction used. Having large or heavy breasts alone may not qualify for Medicare rebates.
“A surgeon can tell from photos whether I qualify.”
No. Item applicability often depends on findings, history, documentation, imaging where relevant, and the full clinical context.
How the Medicare pathway usually works in practice
Documentation of symptoms, history, and initial assessment
Imaging or physiotherapy input where appropriate
Assessment by a plastic surgeon
Clinical suitability and potential Medicare item applicability
Discussion of options, risks, recovery, and costs
What to bring to your GP or consultation: practical checklist
If your concern is post-pregnancy or C-section abdominal wall symptoms
- GP summary of symptoms and timeline
- diagnostic imaging report if already performed
- physiotherapy records or treatment summary
If your concern is loose skin after major weight loss
- GP notes documenting rashes, skin irritation, intertrigo, or skin fold treatment
- record of treatment tried over at least 3 months
- weight history showing major weight loss and later stability
If your concern is large or heavy breasts
- GP summary of neck, shoulder, or upper back symptoms
- record of conservative measures already tried
This does not guarantee that an item will apply. It simply makes the consultation more efficient and makes it easier to assess the clinical situation properly. Online information can help you understand the framework, but formal assessment depends on the exact clinical problem, documentation, examination, and where relevant, imaging.
Frequently Asked Questions
Does Medicare cover tummy tuck after pregnancy?
Sometimes, but not automatically. Medicare item 30175 is for a pregnancy-related or C-section problem in the abdominal muscles with abdominal muscle separation (rectus diastasis) of at least 3 cm on diagnostic imaging, documented symptoms, failed conservative treatment including physiotherapy, and no pregnancy in the last 12 months.
Does a C-section shelf qualify for Medicare?
Not by itself. A C-section shelf, pouch, or post-pregnancy bulge may reflect scar tethering, skin excess, fat distribution, diastasis, or a combination. Medicare item 30175 applies only when the formal Medicare criteria are met.
Does Medicare cover body lift after weight loss?
Sometimes, but not for weight loss alone. Medicare item 30179 applies to circumferential (all the way around) excess or loose skin after significant weight loss where there is an associated skin problem, failed treatment over at least 3 months, interference with daily living, and stable weight for at least 6 months.
What does significant weight loss mean for 30179?
Medicare defines ‘significant weight loss’ as a reduction equivalent to at least 5 BMI units, with weight stable for at least 6 months before surgery.
Does Medicare cover breast reduction in Australia or provide a rebate?
Sometimes. Medicare item 45523 is the main item patients usually mean when they ask this, but it does not apply to every breast reduction. Medicare rebates apply in patients with macromastia, or heavy breasts, causing neck or shoulder pain, and the specific technique of breast reduction.
Does breast size matter for Medicare? Does 45523 require a minimum amount of tissue to be removed?
Medicare rules apply to symptoms and the type of breast reduction procedure being performed, rather than listing a minimum amount of tissue to be removed.
Can Medicare eligibility be decided from photos alone?
No. These decisions depend on symptoms, examination, imaging where relevant, treatment history, and the exact operation being considered.
What should I bring to my GP before seeing a plastic surgeon?
Bring the most relevant records for your situation: imaging if already performed, physiotherapy or other conservative treatment history, documentation of rashes or skin fold treatment if relevant, weight history after major weight loss, and a clear summary of symptoms and how they affect daily life.
Where to go next
If your concern sounds like a C-section shelf or lower abdominal pouch → read:
- C-section shelf or pouch: causes and treatment options
- Tummy tuck / abdominoplasty
If your concern is excess skin after major weight loss → read:
If your concern is heavy breasts with physical symptoms → read:
If you want to understand your own situation properly
A consultation is more useful than trying to self-diagnose from Medicare numbers alone, especially if you bring relevant documentation. In NSW, even where Medicare and health fund rebates may apply, surgery in these categories is typically undertaken in the private hospital setting.
Understanding Medicare item numbers can be helpful, but they do not replace clinical assessment.
If you would like to understand how these criteria apply to your situation, a consultation allows for a more accurate and personalised assessment based on your symptoms, examination findings, and relevant documentation.

For more information
Medicare criteria are defined by the Medicare Benefits Schedule (MBS). Eligibility is assessed according to Medicare Benefits Schedule (MBS) criteria and requires clinical documentation by a qualified medical practitioner. These criteria are strictly defined and regularly audited. For further information, please visit the MBS site or Services Australia. The only way to determine whether a Medicare item applies is through formal clinical assessment based on symptoms, documentation, and examination.
About the Author
Dr Varun Harish is a FRACS Specialist Plastic, Reconstructive and Burns Surgeon in Sydney. His clinical practice includes post-pregnancy abdominal wall surgery (including rectus diastasis repair), body contouring after significant weight loss, and breast reduction for symptomatic macromastia.
In clinical practice, Dr Harish regularly assesses patients seeking advice about Medicare eligibility for procedures such as tummy tuck, body lift, and breast reduction. This includes evaluating whether a patient’s symptoms, examination findings, imaging, and prior treatment align with specific Medicare Benefits Schedule (MBS) item numbers such as 30175, 30179, and 45523.
His approach focuses on distinguishing between cosmetic concerns and medically indicated conditions, explaining how Medicare criteria are applied in practice, and helping patients understand when a rebate may or may not apply based on their individual clinical situation.
This content is written and clinically reviewed by Dr Varun Harish based on current MBS criteria and real-world assessment of patients in Sydney.
Dr Harish is the 2026 recipient of the Dr Ray Hollings Surgical Excellence Award (Northern Sydney Local Health District). He has a strong academic and research interest in plastic and reconstructive surgery, with peer-reviewed publications and ongoing involvement in surgical education.
This article reflects Dr Harish’s clinical experience in assessing patients for Medicare-rebatable procedures and explaining how formal eligibility differs from general online information.
You can learn more about Dr Varun Harish here.
Educational information prepared by Dr Varun Harish FRACS, Specialist Plastic, Reconstructive & Burns Surgeon – Sydney.
Serving patients across the North Shore, Northern Beaches, Inner West and Central Coast.
Last reviewed April 2026.
Read how this site’s medical content is prepared and reviewed
